Where to begin with this tale is a tough one. Of all the jobs I have had, working in the The Northern’s Maternity Unit is going to be one of the places I will forever be most proud of working in. But the why this is, isn’t simple. I’ve worked in Children’s Oncology and a prestigious ICU and so many other interesting jobs When did I even do this? You may ask. Between 2016 and 2022 I have worked two jobs at a time – often with conflicting rosters. A brutal 6 year period where I worked more than full-time hours between these jobs.
This blog entry doesn’t have the space to tell the whole tale of my time in Mat. It is a story of joyful moments and the formation great friendships, framed against tragedy and some of the worst I have seen of humanity. Please, stow your tray tables and fasten your seatbelts, this is going to be a bit of a journey.
5000+ Babies.
Back in April, 2014 I was preparing to return to Melbourne and was wrapping up my work at the now defunct Queensland RCH. I’d been looking to get straight back into work the moment I arrived in Melbourne, seeking opportunities in either hospitals or other healthcare providers. Anything to get me started in a new life back in the city of my birth.
One of the jobs I applied for was with the Casual Employee Pool at The Northern Hospital. One morning while reading in bed I received an email requesting that I attend a 15 minute interview that was due to occur later that week. Being 2 states away I had quite a challenge to this. So I called the contact person to see if I could push it back a bit, and instead she said “Let’s just do the interview now”. The interview went well and I got the job. All while I was still in my PJs.
I don’t wear PJs.
The next month I flew down to Melbourne to start what was a week of induction and training. However, unlike everyone else starting in the casual pool I wasn’t going to be immediately working. While I was there, the person in-charge of the pool asked if anyone wished to apply for an ongoing job in the maternity department. I had never seen someone approach a group like this to fulfil a position, and I with caution disregarded it, feeling that it was clearly a role they had struggled to fulfil with people that worked in other departments, indicating there were big challenges to the job. Besides, I was a male – men rarely work in maternity… right?
It had been a month since the job in Maternity was offered when I finally had finished moving and commenced work on the casual pool. While I went about my last days in Brisbane the through, thoughts of the job kind of ate at me. Why not apply? Something about the offer at the time told me the person in-charge of the casual pool thought I would be good fit. I could shake the feeling that I should have challenged my attitudes and just applied – to see what would come of it.
I approached the pool manager and discovered that they had gone through the application process and found no one suitable. The moment I asked her about the job a look of excitement came to her eyes as a smile stretched across her face. In that moment I felt a sense of dread that I was about to be corralled into something, and nearly regretted showing my interest.
“I tell you what” she said. “Here’s the number of the unit manager, you call her and have a chat” .
So I did.
The unit manager asked me to pop up to the ward and have quick meetup, just to see if I felt the role was right for me. In reality she wanted to get a sense of it I myself was right for the job. After about 10 minutes of talking in the hallway about my experience working in healthcare up to that point, she paused and told me to wait. Within minutes I was ushered by into room where two other department managers and I soon was being interviewed by an impromptu 3 person panel. By the following week I was seated out the front of the department on a desk with a woman named Jess who began showing me the job.
I had only worked a whopping 2 days a casual before picking up ongoing part time permanent work. A fact still seems absurd today.
I became one of the first faces women saw when coming into the the ward, usually in labour or the early stages there-of. While I was hired by the Maternity ward itself, I found myself working far more with the midwives in Birth Suite unit, and the assessment unit positioned just behind it. I quickly bonded with the staff in there, many who were younger and had had far less experience working in healthcare than I did, while many of the older staff seemed to appreciate something else I brought to the role. I also had a lot of involvement with the Special Care Nursery – later re-named the Neonatal Unit.
It wasn’t easy work… ever. In fact, in some of the early days I questioned if I was up to the task and I often rode home on my motorbike feeling utterly exhausted. But as I built relationships around the department things changed and I felt things starting to improv in my work life and felt I was really making a difference. I was asked to be part of the redesign program that the hospital had initiated to look at improving workflows, something that would end up expanded the staffing hours of the role I was working in. When that happened I then took on working in maternity full time. I felt the organisation had trust in me, and I now started to feel very much at home.
By the time I finished working in Maternity in February, 2022 – near 8 years later I can’t say how many babies I’d seen heading out from the ward in the care of their new family. When I stopped working my second job with the ICU in 2019, the estimate was about 5000.
You know what? I never stopped having a peek at them as they came past.
The Trolley Thing.
Anyone that is “friends” with me on Facebook has seen it. Follow me on instagram? You’ve seen it there too… postings about supermarket trollies. (carts in some parts of the USA, Buggy in others, Trundlers in some parts of New Zealand). It’s been a very long running joke that I have shared with staff working at The Northern Hospital, but it didn’t start off entirely as a joke.
Directly across from the hospital is a large shopping complex. For some reason many of the trollies ended up across the road at the TNH (The Northern Hospital) and one morning while riding into work I found a pile of them forming something of an ugly unwanted gateway to the hospital. It was sad to look at it, and I felt that the patients of the hospital deserved to be greeted by something far more dignified than a trash-dump of trollies when they arrived into our care.
So, What does a typewriter/blogger/writer do when he wants something done?
Poetry.
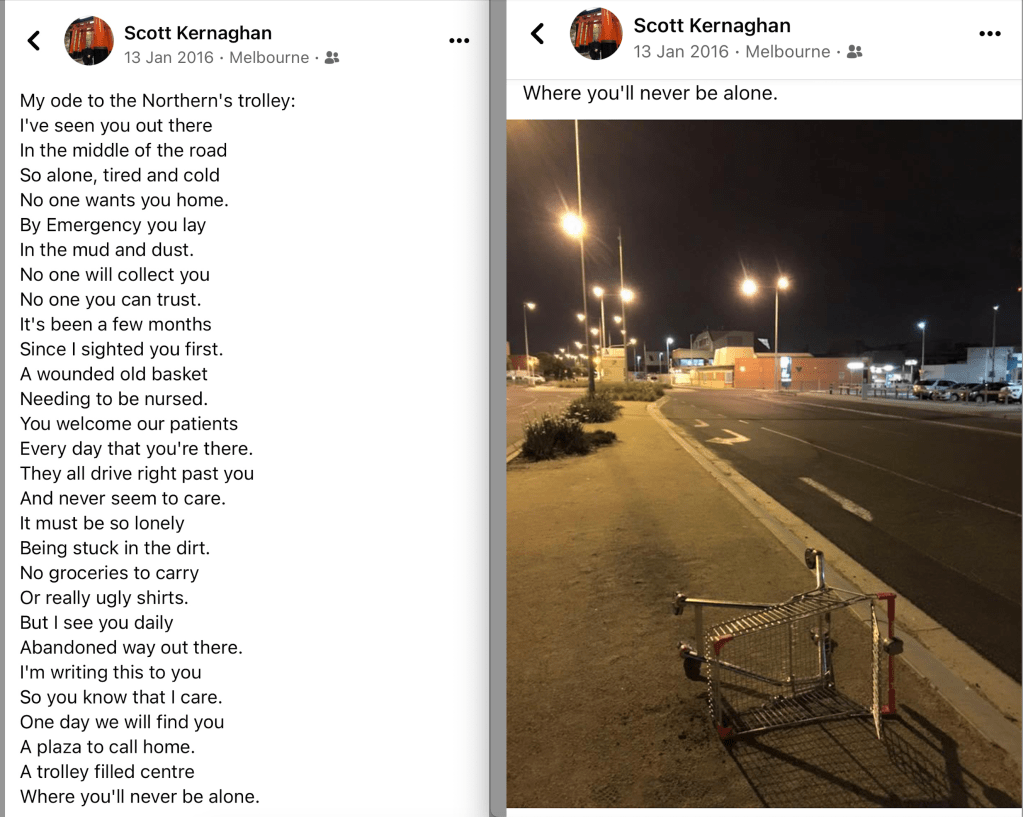
After finishing a shift at 11pm one night I walked out front to see several trollies parked in the usual mess out front of the hospital. I took a photo of one sitting on its side in a traffic island at the hospital’s entrance that had been there for 4 months, and posted it on the shopping complex’s Facebook page with my little poem about that trolley.
The next day the shopping centre came and picked it up. Mission accomplished, right?
Uh.
Well the trollies kept coming, so it became a game where I would take photos, post it and quickly make up a little story about each trolley. Different shops in the complex had different coloured trolleys, all of which lent themselves to becoming characters in the ongoing saga. I introduced “The Red Barrow” and a blue one became “Police Trolley”. Trolleys fallen over into bushes became known as the drunk trollies. Sometimes trollies were seen squaring off for a fight in the car park.
It became a bit of a community running joke at that point. People started posting trolley related jokes on my own Facebook page and co-workers at The Northern even gave me mini trolley gifts. This was fantastic – I felt they really got my sense of humour.
The one thing that eluded me for so long was – why did the trolleys keep coming? I had managed to get the centre to motivate their collection crews to pick them up more often for a while, but they still kept coming. There’s no one single answer for this, but one afternoon I got a bit of an insight that I wasn’t expecting. As I walked out the front door after finishing a shift one afternoon I found a woman pushing a trolley past me – right by the hospital’s front doors. Inside of it was a walking stick, an empty box that had once contained a cheap, slow-cooker and some scrappy bits of fabric.
I stopped and talked to her, and she was very happy to chat. The Northern Hospital has two large mental health inpatient wards and she had recently had a stay in one of them. On previous occasions when she had been discharged she went and stayed with family, however those options had been exhausted now and after her most recent inpatient episode she found she had no where to go to. She had been living behind the hospital, finding makeshift materials to build a shelter somewhere on the hospital grounds. The night before another homeless person took what she had, so she was now using a trolley to collect as many things as she could before that night. The flotsam that was in her trolley was all she had in the world – or at least that she knew of.
As I walked away I felt a sense of grief for her situation. This didn’t explain every trolley that was found on the grounds, but I momentarily felt little bad about making such a joke of these trollies. But then again, I had achieved what I set out to do – bring joy and dignity back into my environment. The homeless woman was teed up with a social worker that afternoon, and located into a shelter near-by.
Paving The Way With Gold –
And Other Acts Of Aggression
One of the most complex issues facing our community socially these days is domestic violence. News and media sites often throw around statements like ‘rising domestic violence crisis’ and ‘post me-tooism’. But these tropes don’t actually help socially as they imply there’s some new shadowy attitude or force that is at play in our society. Often columnists and conservative opinionators like the play it off by blaming the victim – asserting the role of men is so diminished in our world these days that they, we, have lost their masculine identity resulting in this… ‘crisis’.
It’s bullshit. Absolute self-serving dumb-f**kery. Domestic violence, and the will to violence has been here all along. In a world now filled with cameras and quick access to communicating to larger audiences, this violence is no longer remaining behind closed doors and away from the eyes of peers and family. It’s not new. It has always been there, hidden behind suburban fences.
Taking on a role where I dealt with families coming in for care that is entirely focused on achieving the best outcomes for the mother and children, brought this quickly into sharp focus. The insidiousness of domestic violence was there… always there. Being the first person a couple would be in face to face contact with when arriving at the hospital, I often found myself being unwittingly involved in active acts of domestic violence, or the aftermath there of. I have had women debrief onto myself the abuse they had just suffered at the hands of their partners prior to their arrival, their partner still standing next to them fists clenched. Other times they arrived alone, begging to hidden from their abusers.
I was part of a group involved in creating a process that allowed us to allow these women to arrive and be safely cared for, while keeping them hidden on our computer systems so other people around couldn’t search our systems to find their whereabouts. That’s the thing about being a hospital at the centre of a community, sometimes they know other people that they can ask to find out details for you.
But acts of aggression aren’t always so openly presented. When I hear “Men’s Representative/Rights” groups talk about the diminished role of men in our society, I find this frustrating and deliberately ignorant. Aggression in hospitals is unfortunately commonplace, and I noticed a cycle very early on in my time working in Maternity that I came to call “Paving The Way With Gold”. This is aggression that occurs with men who have limited communication tools and skills, trying push for a better outcome for their partner – often with no obvious potential gain other than removing perceived hurdles. The nature of healthcare is slow, considered and methodical. The heightened emotional state around women labouring, sometimes even before that, doesn’t give much scope for the needed patience from partners, sometimes resulting in aggressive acts as they push hard for an outcome.
It is also aggression that could have been avoided by more involvement earlier on in the pregnancy by their partners. While some men like to paint these acts as doing the right thing by ‘their woman’, that claim doesn’t stack up. I have had partners speak and answer for expecting mothers as though they are the only ones that can articulate the woman’s current condition, only to complicate things with their lack knowledge of even basic details. This doesn’t help. Sometimes as partners over asserted themselves and aggression escalated, it made clinicians cautious or reluctant to work with the patient as they bumped against a combative barrier they need to get past.
Typewriters In Maternity
Of course a slipped a few typewriters into Maternity from time to time. One of my favourite ice-breakers when I had new staff coming in to the unit, was to get in early and pop the computer’s keyboard and mouse away from where it would be easily accessed and stick a hastily scrawled sign on the monitor – Sorry, computer broken. Use typewriter to make patient labels.
Of course I used a variety of machines typically around a century old, simply to make the whole thing seem even more absurd. I used a Royal 5 (flatbed), a Smith Premier 10 and of course the Corona 3 depicted above.
That Corona has since been passed to another collector in Japan, a lovely chap by the name John Munroe.
As my time came to a close in maternity, I once again took to the typewriter to bang out another handful of farewell letters. After all, it is a tradition of mine now to do so as I finish at a job. This time I pulled out a trusty Hermes 3K to get the job done. It was the first time in over two years I had typed, and as joyful as it was, there were a few tears shed as I wrote.
Babies in a time of Covid.
For those working in healthcare, Covid has been the prover of one’s soul. When it started, some parts of it I found easier to deal with than others around me did. I’d worked in children’s oncology. I had worked in a major ICU that was constructed to be able to cope with ebola patients, and had considerable training on how to use PPE appropriately in these spaces. Masking up wasn’t a scary prospect to me, but it was to many. It is hard enough trying to communicate with scared staff why you need to mask up in an environment that wasn’t used to such precautions on a day-long basis, let alone dealing with patients and families to whom that this was entirely an alien concept.
Ever tried asking a labouring woman to put on a mask?
Then the lockdown restrictions came in.
In most healthcare settings it is usually the only patient, and sometimes the carer who has ownership of what is happening. With childbirth however, a far larger part of the family and social circle is often intimately involved. Having patients mask up was one thing, but having to tell families they could not come in with the expecting mother to the unit often made me feel like I had become the door-bitch from hell. It is impossible for me to summarise exactly how complicated this time was, and it is a subject I could devote an entire blog to – if not a book.
But Covid brought other fears with it. As Melbourne became the centre of Australia’s largest pre-vaccination outbreak, the restrictions came on hard, and often expecting mothers became fearful that they would be whisked off and locked away somewhere they did not want to be if they simply came in contact with someone that was covid positive. No where was this more prominent than The Northern Hospital that sat central to many of the largest outbreaks.
One of the first questions I would ask of patients coming in was if they had been in contact with someone, had symptoms or were actually Covid positive. Many times I was greeted with anxiety about the question. Sometimes the patient would say no – even though the answer should have been yes. On one occasion I even assisted a patient into their room, only to have them say to the midwife that came in after me that they were covid positive – the fear they would be turned away was so great.
The ‘big’ lockdown in June 2020 brought with it curfew and travel distance restrictions. Being a healthcare worker I simply needed to wave my ID if I was questioned outside of my travel distance or hours, but work provided me with a front-line worker authorisation letter just in case. With my shifts often ending after the curfew times, I frequently found myself driving home in what felt like an alternate universe. No planes overhead, no cars on the roads. police roadblocks set up in ever-changing locations. The world was an inky blackness of withheld activity.
Even simply being able to work became a challenge. Being that I still worked at two different organisations, at one point restrictions came into play dictating who could or could not work between two different hospitals – with the risk of spreading potential infections from one to the other being too great. Fortunately the areas I worked in did not appear on the list of locations that could not work between campuses, but there was plenty of anxiety about me doing so
The stress of it started to take its toll. The hobbies I enjoyed – writing, travelling, collecting – everything became stressful. I packed most of my collection away and found myself withdrawing. It took a toll on my body too, the inevitable results of less activity coming in. Many times I looked at my hands, so red with layers of skin being stripped away with hand-sanitiser every time I touched something. I remember watching the skin strip away as I took a ring off one night, from then being the last time I wore any jewellery for the next two years. The masks marked my face, often deeply on some occasions, but I still wore them every day.
The daily complexities that I had to deal with so often became trivialities to friends that weren’t in healthcare. The “why should I” statements came thick and fast as they ranted at me. All the while in the back of my mind I was forever conscious about some of the horrible outcomes I had seen with not just covid infected patients, but the carers that were infected in a time before we had any vaccine protections. As frontline workers we weren’t just highly exposed to covid, were were also increasingly exposed to anger and outright f**kwittery, that was thrown at us simply because we were the most visible element of the pandemic.
To all my colleagues that made their way through this time, yeah… it was hard. It was f**king hard hey.
Community…
A six months in to my job in Maternity one of the volunteers of the hospital walked into the unit and stopped in front of my desk, where I was talking to a new mother who was leaving the hospital. The volunteer was overjoyed at seeing the woman’s newborn and started to make quite a fuss at newborn baby in her arms. Having never met me before, wrapped up in the moment the volunteer turned to me with a beaming grin from ear to ear, and started telling me about how amazing and beautiful that baby was. With the new mother awkwardly smiling back, unsure how to deal with this situation she looked at me anxiously. I hesitated to respond while I carefully mulled over my thoughts, but the volunteer took that hesitation differently “Oh, you would never get it. You’re a man” She dismissed with a flap of her hand and a shrug of her shoulder.
“I’ve seen at least thousand of babies. I just have a job I need to get done”. The volunteer bid farewell to the new mother and walked away.
There’s often a sense of joy we experience in the community about the birth of a new child and we often feel a wanting to take part of that. It’s an experience that we sometimes forget happens at the point where the parents of that child are forming an important bond, and there’s a lot of stress as people come in and out of the child’s life having their own moment of joy with that child.
It was an immense privilege working in Maternity. Not just for the patients I got to interact with, but because of the people I worked amongst. I have walked away from Maternity with some great friends, people who continue to make my world better every day. It was an experience that had many lows as much as highs, but shifting out of my comfort zone brought many wonderful people permanently into my life, and given me some beautiful memories and experiences.
The work was hard, but it was never too hard when you cared for the people you worked with.
At the end of 2021 I had a sense that in the next year I would have to give up my job at Maternity as working between the two hospitals had become increasingly hard. With this in mind I decided I would end the year by producing a small forrest of 3D printed Christmas trees to be displayed across the front desk, along with a snow-family that I took care to print. These weren’t the store-bought decorations the everyone had seen a thousand times.
It’s hard to see it, but the snow-mother is printed with a translucent material and inside is a tiny snow-baby.
This wasn’t the last 3D printed tribute I produced for my out-going ward. As I wrote my farewell letters I designed and produced a sculpture to say thank, which my now former team-members have since put on display at the front counter where everyone that comes in can see it. It was a job I had loved for the past 8 years, and am immensely proud of. I had helped a lot of people working there, and always felt like I belonged. It was beautiful, and I can’t capture in a single blog entry all of the things I experienced working there, now the deep love and appreciation I have for the people I had worked and cared for patients with.
As I walked out at the end of my last shift, I couldn’t help but feel I had unfinished business, as though some day I would be back to The Northern Hospital.
Maybe.
Maybe I need to just write a book.








Well, you have had a bit of a life since your last post! 😀
Glad that you found much satisfaction within the difficulty of a very demanding career (in an even more demanding time). Here’s to hoping your New Year brings work that allows you a bit more free time to enjoy your typewriters and maybe even post a bit more – get that platen even filthier. (:
LikeLike
The passion is slowly coming back. I’ll get there!
LikeLike
I love the practical joke with the Corona, and the notes you typed on the Hermes — good workplace uses of our favorite machines. You have done so much and lived a lot in Maternity. Write a book about it!
LikeLiked by 1 person
It’s something I have started working on. Can’t hurt to just get some of it down on paper and see what comes of it.
LikeLike
Great post. Thanks for sharing some of the stresses and craziness of that strange bundle of years.
LikeLiked by 1 person
Thank you! There’s a lot I could post about those years. But that may have to be for another day.
LikeLike